Postpartum Gut Issues: Why They’re So Common (and What Actually Helps)
About the Author: Taylor Stolt is an award-winning Functional Medicine Dietitian, women’s health expert, and founder of Plate and Canvas, a virtual practice that has helped over 700 women address hormone and gut issues through comprehensive testing and personalized protocols. Her team helps women heal in a way that supports real life, not perfection, so clients can feel like themselves again without extremes or restrictive diets.
If you’ve noticed digestive issues after having a baby, you’re not alone.
We regularly work with women months (or even years) postpartum who were told everything is “normal”, yet things still don’t feel right.
In this blog post we’ll cover:
The four main reasons postpartum digestive issues happen
Which symptoms are normal, and which aren’t
The two tests we recommend
How to support postpartum digestion naturally
Four Main Reasons for Postpartum Gut Issues
Postpartum digestion is rarely affected by just one thing.
In most cases, several root causes are involved at the same time, including:
Hormone shifts
Pelvic floor changes
Nervous system dysregulation
Sleep deprivation
Microbiome disruption
Pain medications
Changes in hydration
Changes in eating patterns
While many factors can be involved, these are the four most common drivers we see.
1. Hormone Shifts
During pregnancy, high progesterone slows digestion (this is why constipation and reflux are common).
After delivery, estrogen and progesterone drop abruptly, and that sudden shift can disrupt gut rhythm, stool consistency, and sensitivity.
Breastfeeding, sleep loss, and stress create even more disruption via the gut–brain connection.
This can make digestion more reactive or unpredictable, even if your diet hasn’t changed much.
2. Microbiome Disruption (A Big One)
Pregnancy, labor, antibiotics, and stress all shift the gut microbiome.
We often see postpartum women with:
Reduced “good” commensal gut bacteria
Overgrowth of gas-producing and/or inflammatory gut bacteria
Increased gut inflammation
Low levels of digestive enzymes
These imbalances can drive bloating, acid reflux, heartburn, upset stomach, constipation and diarrhea, especially if you had digestive symptoms before pregnancy.
3. Pelvic Floor Changes (Even If You Had a “Normal” Delivery)
Your pelvic floor plays a huge role in bowel function, not just bladder control.
After pregnancy and delivery, your pelvic floor muscles may be weak, tight, or poorly coordinated. Nerves involved in bowel control can be irritated or stretched. Pain or fear of straining can also lead to unconscious muscle guarding.
This can happen even without tearing or a dramatic birth experience!
These pelvic floor changes can lead to:
Constipation
Feeling “blocked”
Incomplete emptying
Stool urgency or leakage
4. C-Section and Pain Meds
If you had a C-section:
General anesthesia temporarily slows gut movement
Opioid pain meds worsen constipation
Abdominal surgery changes pressure and coordination
Gas pain, bloating, and delayed bowel movements are very common early on, but in some women these issues linger without targeted support.
Normal Early Postpartum Gut Symptoms
In the first 2–6 weeks after birth most women experience these normal, self-resolving issues:
Delayed first bowel movement (up to 3–4 days), then gradual return to regularity
Constipation with hard stools, straining, or incomplete emptying
Gas and bloating
Stool urgency or loose stools
Mild hemorrhoids: itching, small tender lumps, or bright-red streaks on toilet paper
Discomfort with the first few bowel movements, easing as healing happens
These symptoms should trend better with time and shouldn’t linger for more than 5-6 weeks.
When Symptoms Are Worth a Deeper Look
Digestive changes are expected in the early weeks after giving birth.
But for some women, their symptoms don’t fully resolve. They linger, cycle, or slowly worsen over time.
These are patterns we most often see in women who benefit from functional medicine support:
Constipation that persists for months, not just weeks
Bloating or stomach distention that feels disproportionate to what you’re eating
Gas, discomfort, or stool changes that fluctuate without a clear trigger
Alternating constipation and loose stools
A sense that digestion never quite “returned to baseline” after pregnancy
Symptoms that temporarily improve, then come back again
Why We Use Testing From the Start
Because postpartum gut issues are so multifactorial, guessing rarely works.
One of the biggest frustrations we hear from postpartum women is that they’ve already tried everything.
More fiber. Probiotics. Magnesium. Cutting dairy. And nothing seems to fully help.
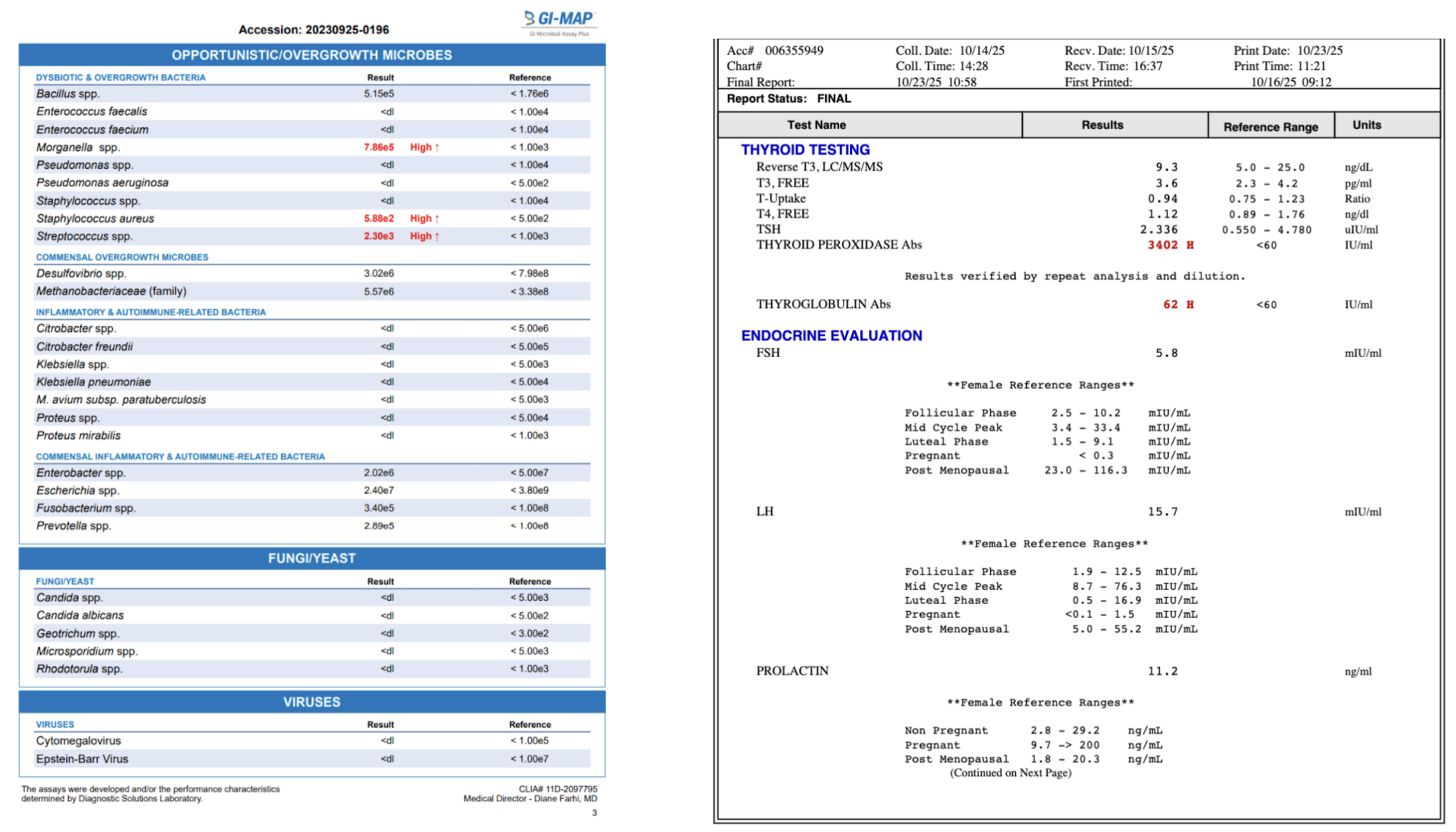
Rather than guessing and hoping something works, we use comprehensive bloodwork and a GI MAP stool test to understand what’s driving your symptoms.
These two tests help us identify:
Gut inflammation
Bacterial or fungal overgrowth
Poor digestive enzyme production
Thyroid issues and nutrient deficiencies affecting motility and healing
Gut–hormone interactions
This allows us to be targeted and efficient - so you’re not eliminating foods you don’t need to eliminate, or taking supplements you don’t need.
After working with 700+ women, we’ve found that postpartum gut issues are rarely “just part of motherhood.”
There’s always a root cause. And once we know what that is, healing becomes much more straightforward.
How to Support Postpartum Digestion Naturally
1. Targeted Nutrition
Our nutrition recommendations vary client to client but we often incorporate:
Gradual increases in gentle fiber-rich foods
Hydration with both water and electrolytes
Mineral-rich foods based on deficiencies
Probiotic-rich foods based on stool test results
Supporting digestion based on your gut pattern
2. Hormone and Metabolic Recovery
After birth, your body is recalibrating multiple systems at once: reproductive hormones, thyroid, stress hormones, blood sugar, and nutrient stores. All of these directly affect digestion.
Low thyroid can slow motility.
Blood sugar swings can worsen nausea, reflux, and urgent trips to the bathroom.
Low iron, magnesium, or zinc can impair gut function and digestive enzyme production.
Inflammation can keep the gut hypersensitive.
This is why we don’t look at the gut in isolation.
Comprehensive bloodwork helps us assess hormones, thyroid function, inflammation, nutrients, blood sugars, and more, so we can support the whole body and bring your gut back into balance.
3. Nervous System Regulation
Your gut listens to your nervous system.
Postpartum sleep loss, anxiety, and mood disorders can all amplify gut symptoms.
Supporting digestion means supporting:
Healthy cortisol rhythms
Sleep quality (so the sleep you get really counts)
Balanced neurotransmitter production
Vagus nerve regulation
Feeling heard and supported in the healing process
Nervous system balance can be achieved through targeted nutrition, lifestyle support, simple breathing exercises, and supplements when needed.
4. Restore Pelvic Floor Function
Pelvic floor physical therapy isn’t just for bladder leaks or pain with sex.
It can also help with constipation, incomplete emptying, gas trapping, urgency and leakage by improving muscle coordination and nerve signaling.
We regularly refer clients to pelvic floor physical therapists we trust and we see meaningful improvements when gut and pelvic floor care are addressed together.
Final Thoughts
Postpartum digestive issues are common, but that doesn’t mean you have to live with them.
If you’re months (or years) postpartum and still dealing with symptoms, it’s not a failure – it’s a signal.
And with the right support, you can heal.
You can learn more about Plate and Canvas and apply to work with them here: https://plateandcanvas.com/1-on-1-consultations